How Does Pressure Cause Tissue Damage - Part Two
A long time ago, in a blog post far, far away, I talked about how pressure causes damage to horses. In that post, I only talked about how pressure impeded blood flow, leading to low oxygen levels, which, over time, damage tissue. But I left that post with the comment that there are other factors that contribute to damage. Here is a very short summary of some of what we know now, and since I did the research a long time ago in a place far, far away, there may very well be more information available now. But here’s something to get those of you interested started in your research.
Lack of oxygen
Did you know that different tissues respond differently to different types of trauma? What affects one tissue type quickly doesn’t affect others as soon? It takes more pressure to close blood vessels in muscle than it does in skin and subcutaneous tissue, so when we measure pressure at the skin, it may or may not be affecting oxygen levels in the muscle. And in testing, you can have complete ischemia (no oxygen available) to muscle for two hours without permanent damage – provided nothing else is happening. The cells will recuperate and be fine after that length of time. In fact, one study showed it takes five hours for muscle to quit functioning just because of lack of oxygen. Yet we know that muscle atrophy happens to horses with far less than five hours of complete lack of oxygen. So what gives?
Lymphatic drainage and reperfusion injury
Well, there are other things that cause damage as a result of pressure than just lack of oxygen. The pressure that stops oxygen coming in via small blood vessels also closes off lymphatic drainage, so all the waste products of the cell are not removed. They stay in place and can be toxic to the cells themselves. Then you can get what is called reperfusion injury or reactive hyperemia as blood flow is reestablished and the capillaries open up wide. All the toxins produced, including free radicals, are then available to cause tissue damage locally before being removed. Some people even think that this reperfusion phase is more damaging than the ischemic phase. This is why in practice, it is best to loosen your cinch and let the saddle sit for a while before removing it rather than just coming in and taking the saddle off all in one fell swoop. Seems the old cowboys learned from experience what scientific studies are just now discovering the reasons for.
Tissue distortion, friction and shear
We know that the body can actually withstand immense pressures without damage. This is seen in deep sea divers where there the pressures from the water on the entire body are super high. But the key is that the pressure is equal everywhere on the body. It is when there are uneven pressures – pressure in one area and not another – where tissue distortion occurs, and that causes damage directly to the cells. Muscle is especially susceptible to this kind of damage compared to things like skin. When cells are harmed by high enough pressure that the cell membranes tear, the damage is irreversible. This pressure can be directly down on cells, but it can also be through friction and shear. Shear pressure results when one layer of tissues slides relative to another. This happens in bed ridden patients where they are moved by dragging them against their beds. The skin layers have friction that tends to hold them in one place while the underlying tissues are moved more quickly, causing shear pressures between the tissues.
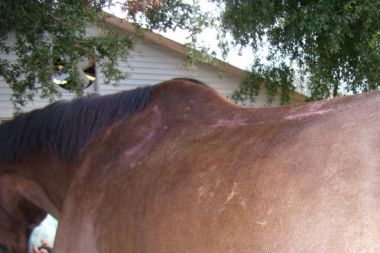
Shear effect on horses
 |
 |
This also may explain why our more A shaped horses, those tall withered TBs and warmbloods, seem to develop atrophy behind the shoulder blades so commonly. They will have much more shear pressure in that area because the saddle is relatively more vertical compared to our broader backed QH type horses. Pressure between saddle and horse will tend to pull down on the skin in the wither area, creating shear pressure. We also need to reconsider the use of synthetic pads that are tacky or sticky and are supposed to “hold the saddle it place”. Under the saddle, these will move the skin, under pressure, relative to underlying tissues, and can cause damage.
But I think that the biggest area of concern with shear is movement. Think about what happens when the shoulder blade moves underneath a saddle sitting on top of it. In this case, the skin isn’t moving. It is solid under the saddle. But the bone underneath that skin is moving relative to the skin and likely creating shear pressure between bone, muscle and skin. No wonder the muscle is damaged when the saddle is placed on top the shoulder blade! Yes, muscles underneath a saddle that is in the correct position, with the front of the bar tip just behind the shoulder blade of the horse, will also move, but they don’t move positionally relative to the saddle. They contract and relax underneath the saddle. They don’t shear against the saddle like what happens when the shoulder blade moves relative to the saddle. Proper position is vital to preventing shear damage.
Combinations make it worse
There are many different things that cause tissue damage, and the different factors cause more or less damage to different tissue types. In fact, the pressure that ends up causing damage has a very wide range in testing, showing variables not just in tissue types but in different tissue samples, and therefore it differs between horses as well. But one thing that is mentioned in a lot of the research is that the combination of lack of oxygen and tissue deformation that results in the most damage most quickly. Where ischemia by itself might be OK, and tissue deformation by itself might be OK, together, they result in irreversible damage much earlier. And while, in the lab, scientists can separate out the different types of trauma, in real life, all these things can happen at the same time under our saddles.
It all comes back to the 3 Ps…
Thinking about how this applies to saddle fit – high pressures cause lack of oxygen, so keep the Pressures as low as possible. This can be done with increasing surface area and preventing high pressure areas – no Poking. We need to prevent tissue deformation and cell damage from really high pressure areas – Poking, even intermittently, and from friction and shear pressures caused by rough or sticky materials under the saddle. And we must prevent friction and shear pressures between tissues under the saddle by having it in the correct Position. It makes sense that damage occurs from multiple factors that exacerbate each other. Keeping the basics correct will alleviate each factor in its own way and prevent the combination of factors doing damage.
Information gathered from the following references:
(1) Ferguson-Pell, Martin, Hagisawa, Satsue, Biochemical changes in sweat following prolonged ischemia, 1988, Journal of Rehabilitation Research and Development, Volume 25, #3, 57-62
(2) Polliack, Adrian, Taylor, Richard, Bader, Dan, Analysis of sweat during soft tissue breakdown following pressure ischemia, 1993, Journal of Rehabilitation Research and Development, Volume 30, #2, 250-259
(3) Taylor, Richard, Polliack, Adrian, Bader, Dan, The analysis of metabolites in human sweat: analytical methods and potential application to investigation of pressure ischaemia of soft tissues, 1994 Ann Clin Biochem 31:18-24
(4) Linder-Ganz, Eran, Engelberg, Santiego, Scheinowitz, Mickey, Gefan, Amit, The analysis of metabolites in human sweat: analytical methods and potential application to investigation of pressure ischaemia of soft tissues, 2006, Journal of Biomechanics 39 2727-2732
(5) Loerakker, S, Stekelenburg, A, Strijkers, G.J., Rijpkema, J.J.M., Baaijens, F.P T., Bader, D.L., Nicolay K., Oomens, C.W.J., Temporal effects of mechanical loading on deformation-induced damage in skeletal muscle tissue 2010, Annals of Biomedical Engineering, Vol 38, #8 2577-2587
(6) Stekelenburg, Anke, Strijkers, Gustav J., Parusel, Henry, Bader, Dan L., Nicolay, Klaas, Oomens, Cees W. Role of ischemia and deformation in the onset of compression-induced deep tissue injury: MRI-based studies in a rat model. 2007, Journal of Applied Physiology 102: 2002-2011
(7) Bouten, Carlijn V., Oomens, Cees, W., Baaijens, Frank P., Bader, Daniel L., The etiology of pressure sores: skin deep or muscle bound? 2003 Archives of Physical Medicine and Rehabilitation May 2003
(8) Gefen, Amit, 2009 Reswick and Rogers pressure-time curve for pressure ulcer risk part 2 Nursing Standard 23, 46, 40-44
(9) Gefen, Amit, Farid, Karen J., Shaywitz, Ira, 2013 A Review of Deep Tissue Injury Development, Detection and Prevention: Shear Savvy,2013 Ostomy Wound Management 59(2):26-35
(10) Loerakker, Sandra, Aetiology of Pressure Sores, 2007 University of Technology Biomechanics and Tissue Engineering
